Parathyroidectomy Treatment in Pune - Dr. Jaisingh Shinde
Successful parathyroidectomy requires an understanding of both the anatomy and the embryology of the parathyroid glands. The parathyroid glands arise from the dorsal endoderm of the third and fourth branchial pouches. The vast majority of patients have a total of 4 parathyroid glands: 2 superior and 2 inferior.
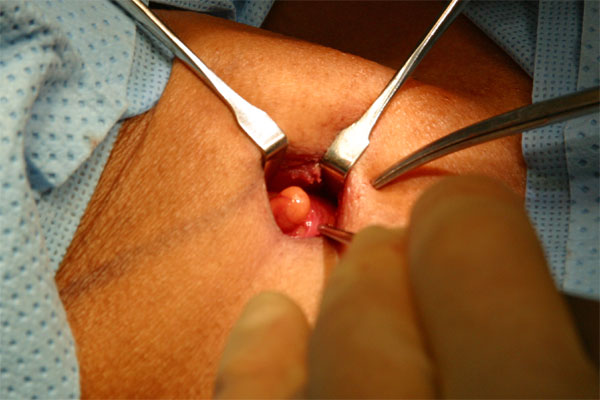
The inferior parathyroid glands, which arise from the third branchial pouch, initially migrate with the thymus until they separate to take their final position, usually at the level of the inferior pole of each thyroid lobe. The superior parathyroid glands (see the image below) arise from the fourth branchial pouch, follow the migration of the ultimobranchial bodies, and usually take their final position along the posterior part of the middle third of each thyroid lobe. The superior parathyroid glands show less anatomic variation than the inferior thyroid glands do.
Historically, patients with primary hyperparathyroidism presented with symptoms related to the effects of PTH on the bone and kidneys. However, with the advent of routine blood screening tests, most patients today are asymptomatic. Currently, only 10-20% have renal stones, and very few have osteitis fibrosis.
Although patients may be referred with nothing more than elevated calcium and PTH levels, further questioning often reveals that they have nonspecific symptoms such as fatigue, musculoskeletal pains and aches, depression, constipation and abdominal discomfort, and decreased memory. These patients may be more accurately described as minimally symptomatic, rather than asymptomatic. Many of them will derive symptomatic benefit from parathyroid surgery, though such benefit cannot be guaranteed in advance.
The diagnosis of primary hyperparathyroidism requires, minimally, an increased serum total calcium level with an increased intact PTH level—or, at least, an inappropriately high normal PTH level. Serum calcium levels can fluctuate somewhat over time, but patients with primary hyperparathyroidism should have a documented increase in serum total or ionized calcium sometime during the course of the condition.
Parathyroid surgery is contraindicated in patients with familial hypocalciuric hypercalcemia (FHH). Patients who have this disorder can present with elevated calcium and PTH levels, mimicking the serum biochemical characteristics of primary hyperparathyroidism. However, FHH is not treated surgically.
In patients with FHH, 24-hour urine calcium excretion is lower than expected in comparison with the serum calcium level. The ratio of 24-hour urinary calcium to creatinine clearance is usually lower than 0.01 in these patients, whereas it is typically higher than 0.01 in patients with primary hyperparathyroidism. In addition, FHH patients typically have normal or mildly elevated PTH levels. Calcium excretion over 24 hours is less than 100 mg in 75% of FHH patients but usually more than 200 mg in patients with primary hyperparathyroidism.
Thiazide diuretics and lithium excess can cause elevated PTH and serum calcium levels, mimicking primary hyperparathyroidism. Therefore, it is important to consider these medications when taking a history and to carry out further investigation if necessary before proceeding with surgery.